31 Mar HRH2030 Assessment of Ethiopia’s Health Extension Program Builds Evidence for Substantial Social Returns on HRH Investments
In one of the first studies to globally measure the social returns of a community health program, HRH2030 has found that Ethiopia’s community-based health extension program has yielded a return of between $1.54 and $3.26 for every dollar invested, indicating that the HEP’s economic benefits exceed Ethiopia’s investment in the program. Benefits from the program were estimated across the following domains: equity, empowerment, employment, and productivity.
Background
Ethiopia’s community-based health extension program (HEP) was launched in 2004/2005 to improve access to health services, especially in rural and medically underserved areas. Through the national HEP, community members, mostly women, are selected to undergo training to become health extension workers (HEWs), which are equivalent to community nurses, and are then employed on the government’s payroll to provide promotive, preventive, and selected curative services with special attention to women and children in rural areas. Through considerable investments since the program’s initial launch, the HEP now has more than 42,000 HEWs deployed throughout the country and has become one of the world’s largest community health programs.
While the health benefits of investing in community healthcare are increasingly known, there has been little analysis about their impact on inclusive economic growth. Traditional return on investment studies only show monetary returns from capital investments and their contributions to health service cost savings. To fill this gap, HRH2030 conducted a study of the health, social, employment, and equity returns associated with increased health service utilization to estimate the social return on investment (SROI), especially for underserved and hard-to-reach populations, from the HEP.
Methodology & Findings
The HRH2030 study focused on the regions of Tigray, Oromia, the Southern Nations, Nationalities, and People’s region (SNNP), and Amhara, where 1,289 HEWs had been deployed by the end of 2005. By 2017, that number had grown to 37,949 HEWs in the four study regions (with a total of 42,336 HEWs deployed in-country). Six different interview tools were developed to collect data to estimate the initial cost and implementation cost of the health extension program. Personnel, recurrent, and capital costs were estimated for the initial investment in the HEP as well as over a 10-year span from 2008 to 2017. Twenty-three (23) clinical activities and six non-clinical activities including the prevention of mother-to-child transmission (PMTCT) of HIV were identified as part of the HEW package of services. The contribution for delivering these services was estimated for HEW as well as non-HEW service providers. Maternal, child, and newborn lives saved for the 23 clinical and six non-clinical services were estimated at the regional level for the period 2008 to 2017. Benefits from the program were estimated across the following domains: equity, empowerment, employment and productivity. All costing and benefit components were utilized to calculate a ROI for each region.
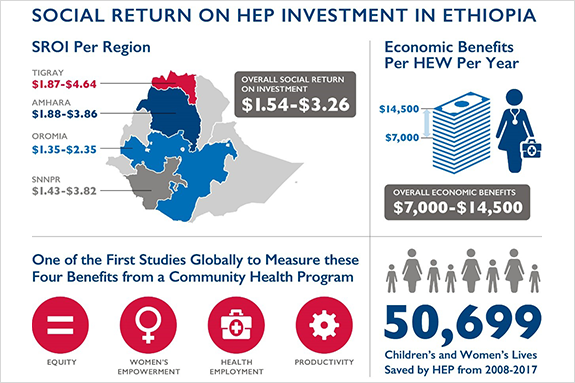
The social return on investment in HEP is between $1.54 and $3.26 for every dollar invested and greater than one in all four regions, indicating that the HEP’s economic benefits exceed Ethiopia’s investment in the program. The highest returns are shown in Tigray ($1.87-$4.64) and Amhara ($1.88-$3.86) and lower returns in SNNP ($1.43-$3.82) and Oromia ($1.35-$2.35). HEP produces substantial economic benefits of almost $7,000 to $14,500 per HEW per year. The higher estimates are based on the value of a statistical life, which is a more appropriate valuation of economic benefits in low and middle-income countries. Productivity benefits, derived from lives saved, make by far the largest contribution with about $4,000 in economic value, except in Oromia, where the economic value is about $2,000 per HEW per year. Second to productivity gains, equity benefits are the next highest contributor, with about $2,000 or 30% of total benefits per HEW per year. Empowerment and employment benefits amounted to about $500 per HEW per year. The study also showed that across all categories of clinical and non-clinical services, a total number of 50,699 maternal and child lives were saved by HEP between 2008 and 2017. This included 2,500 lives saved for PMTCT. These results show that the HEP, while producing substantial economic benefits in Ethiopia, is also having important impact on maternal and child health.
Conclusions
This is the first study in Ethiopia to examine the social return on investment in its HEP, and one of the first studies globally to estimate benefits of equity, women’s empowerment, health employment, and productivity of a community health worker program. While initiating and implementing the national program has been an expensive endeavor, it can save at least 7,000 children’s lives every year at its current level of implementation in well-performing regions and even more with improved coverage for some key interventions. These estimates include about 300 lives saved per year for PMTCT, which is the only HIV-related service provided by the HEWs in the four regions in the study. Ethiopia faces a concentrated HIV epidemic that is mostly clustered in urban centers where HEWs are currently not concentrated geographically. In a generalized HIV epidemic setting a new cadre of community nurses similar to HEWs would be expected to have a much more substantial involvement in HIV treatment and care with much greater health and economic benefits.
Thinking about an application of this methodology beyond Ethiopia, this study shows that in low-income settings, the SROI calculation can extrapolate broader societal values associated with the increased health service utilization, hence emphasizing the social dimensions of the economic return.
Access the full report here. Access the two-page brief here.





